This article was originally published in Fierce Pharma.
In the shift toward value-based care, more payers are outsourcing the management of specific therapeutic areas to third-party specialty benefit managers (SBMs). These companies help payers manage high-cost, high-complexity disease states by leveraging provider networks and making coverage recommendations intended to improve outcomes and lower cost.
Unlike PBMs, which support employers and MCOs in managing prescription drugs and formularies, SBMs are centered on improving the care experience for patients and providers through specialization. Depending on the indication and patient population, SBMs may offer complex care management services, member and provider education, and care pathways development. Typically, they drive volume to less expensive cost-of-care settings and high-performing specialists within their network, often contracting at lower rates.
What does the growing prevalence of SBMs mean for pharma companies? To find out, MMIT’s Biologics & Injectables Index team conducted research with 35 payers covering 116 million commercial lives. We found that payers representing almost half of those lives (44%) are already engaging with third-party specialty benefit managers for at least one therapeutic area.
Let’s dive into the data to better understand the implications of this trend for manufacturers.
The Wide-Ranging Impact of SBMs
Six therapeutic areas in particular—mental health, neurological disorders, diabetes, oncology, immunology and rare diseases—are significantly impacted by the use of SBMs. For each area, at least 74% of the 50.5 million commercial lives covered by these payers is under SBM guidance. The majority of surveyed payers (12 of 17) contracting with SBMs are using their guidance in multiple areas, which is reflected in the percentage of commercial lives impacted (Figure 1).
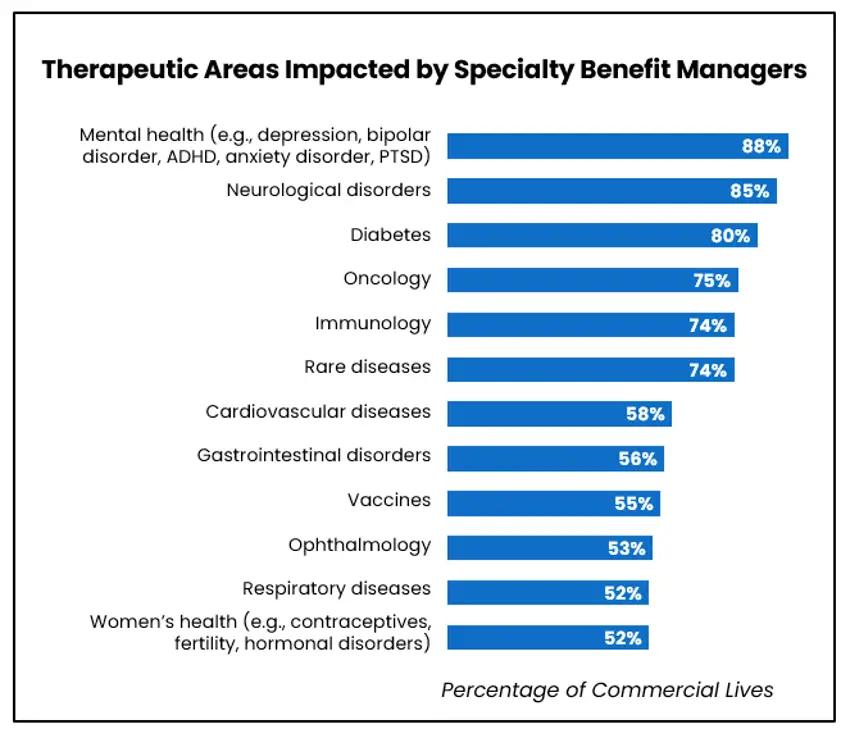
Most payers using SBMs anticipate the percentage of lives influenced by these services to remain constant over the next year. While most payers in this group are not planning to expand their SBM engagement, payers representing 29% of commercial lives do plan to use SBM services in additional therapeutic areas, most notably respiratory diseases and ophthalmology.
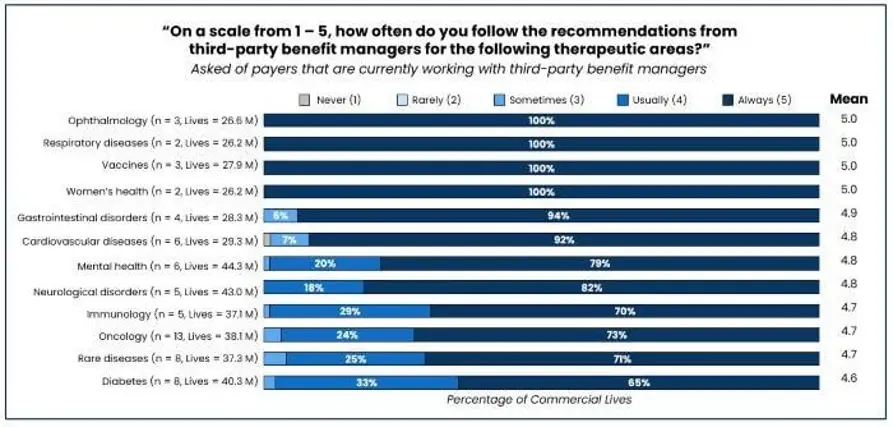
But how dependent are payers on the recommendations of these third-party SBMs? While the number of payers engaging with SBMs varies per category, adherence to SBM guidance is uniformly high across the board. Across the top twelve indications impacted by SBM contracting, the majority of payers say they “always” follow SBM recommendations (Figure 2).
In half the categories, payers representing 18% to 33% of commercial lives say they “usually” follow SBM recommendations, but few payers in any category say they “sometimes” or “rarely” do. Clearly, these payers are quite comfortable relying on the specialized expertise of SBMs.
Payer Perception of the SBM Cost/Benefit Ratio
Overall, payers using SBMs are pleased with the results, and more than two-thirds say the benefits outweigh the cost. Payers representing 96% of commercial lives report that SBMs are helping them achieve greater cost savings, and payers representing 89% of lives say more members are receiving clinically appropriate care. Payers representing ≥72% of commercial lives say that relying on SBM expertise improves member outcomes, reduces risk, and frees up their time and resources.
For payers that aren’t currently using SBMs, cost does not seem to be the deciding factor. Of this group, payers representing 83% of commercial lives cite uncertainty about whether SBMs would actually improve outcomes as a primary reason for not engaging, while payers representing 79% of lives say they have no need to outsource for this function. The belief that SBMs are too expensive was only cited by payers representing 35% of lives.
As payers practicing in-house benefit management take note of the reported advantages of SBMs, the number of payers using these services will likely climb. If payers can reduce administrative burden while cutting costs and improving outcomes, the appeal of outsourced specialty management will be difficult to resist.
Improving Access Depends on Greater SBM Awareness
From pharma’s perspective, the increased influence of SBMs across therapeutic areas is concerning, as SBMs are not typically included in their analysis of the players impacting access. According to our research, the overwhelming majority of payers—representing 93% of commercial lives—acknowledge that utilizing SBMs “typically results in more restrictive policies.”
If payers are almost always following SBM recommendations in these key categories, and these recommendations are more likely to be restrictive, then pharma companies need to ensure that SBMs see the clinical and financial value of their therapies. Manufacturers should work to identify key SBM decision-makers and understand how their management recommendations are determined.
Over the next few years, learning how to identify, approach and persuade these SBMs will become a much larger part of pharma companies’ launch plans and market access strategy. Manufacturers in therapeutic areas with high SBM adoption might need to consider contracting with these companies for preferential access, including formulary placement and medical policy and care path inclusion.
By monitoring SBM/payer alignment along with traditional market access data like coverage, restrictions and pathways, manufacturers can improve patient access to their therapies.
For insights into payers’ relationships, geographic reach and other attributes, learn more about MMIT’s Payer Landscape solution.








