This article was originally published in PharmExec.
At age 19, my stepson has run the gamut of therapeutic options—combination therapies, cognitive behavioral therapy, you name it—for treating his attention deficit hyperactivity disorder (ADHD). After 10 years of searching, we have yet to find a treatment that truly works for him.
However, there’s one option that we haven’t tried: prescription digital therapeutics (PDTs). More specifically, an app-based video game called EndeavorRx. The game, which was approved by FDA in June 2020, is a first-of-its-kind treatment that uses stimuli and motor conditioning to target areas of the brain that control attention function. And the results are impressive: 68% of parents reported improvement in ADHD-related impairments after two months of treatment.
This app could be a game-changer for my stepson and thousands of children just like him. However, despite clearly demonstrated clinical efficacy and very few reported side effects, he can’t use EndeavorRx to treat his ADHD. Why? Because our health insurance doesn’t cover it.
The Missed Opportunity
PDTs are designed and tested much like traditional prescription drugs, but rather than swallowing a pill or taking an injection, patients receive cognitive therapy through software. In addition to ADHD, there are FDA-approved PDTs available for treating substance use disorder, irritable bowel syndrome, PTSD, insomnia, autism, and more.
Yet despite the many FDA-approved options on the market, widespread coverage is sorely lacking: Today, less than half of payers (25%) say that they are willing to cover PDTs, according to MMIT’s recent survey of 16 payers. What’s more, 76% of respondents rated PDTs as a low to moderate priority.
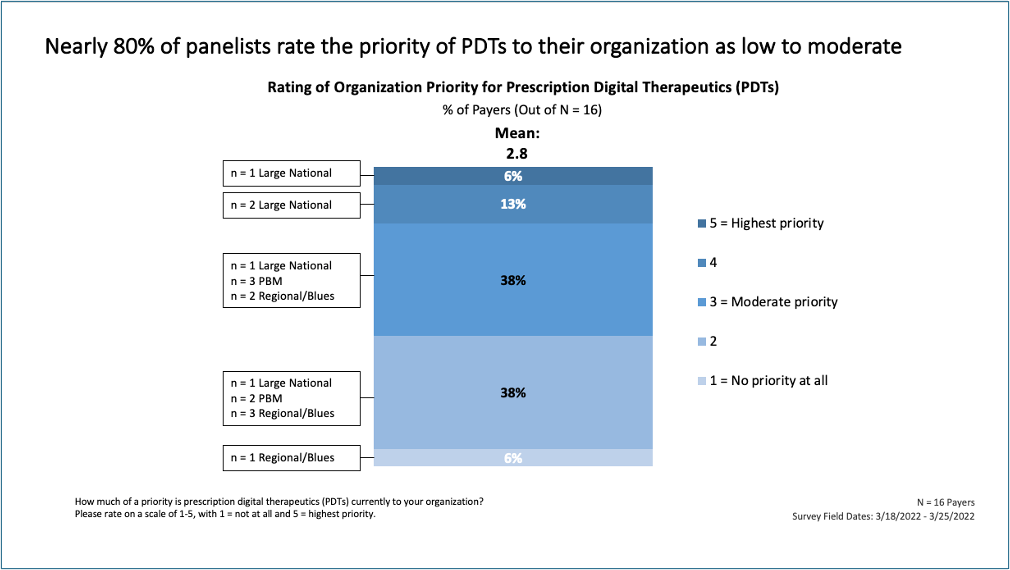
When asked what was holding them back from embracing these therapies, the respondents cited uncertainty around cost savings and disbelief that these technologies can actually hold up to their medical claims. Overall, most felt that PDTs have yet to prove their real value.
“Convenience is not something we are willing to pay for,” said a respondent from a large national plan. Another respondent from a regional plan stated bluntly, “In general, we haven’t found clinical value in the few things that were reviewed, so [there] hasn’t really been a need to go any further.”
Another revealing finding is that 88% of respondents claim that the most important attribute in the review of a new PDT is clinical outcomes. But if that’s the case, then why are payers reluctant to cover so many of the FDA-approved PDTs on the market?
Take EndeavorRx: Despite its impressive product profile, MMIT research shows that Anthem has denied coverage because it isn’t considered medically necessary, and Aetna refers to it as experimental and investigational.
Or consider reSET-O, an app that leverages cognitive behavioral therapy to treat opioid use disorder. In clinical trials, 82% of patients with opioid use disorder who added reSET-O to their program stayed in treatment vs. 68% of patients who did not. However, despite the demonstrated benefits, UnitedHealthcare states that the treatment is unproven and not medically necessary.
These findings are disappointing—not only for me, but also for the many families dealing with chronic issues that could be eased via these new technologies. And unfortunately, coverage is crucial.
The Road Ahead for Manufacturers
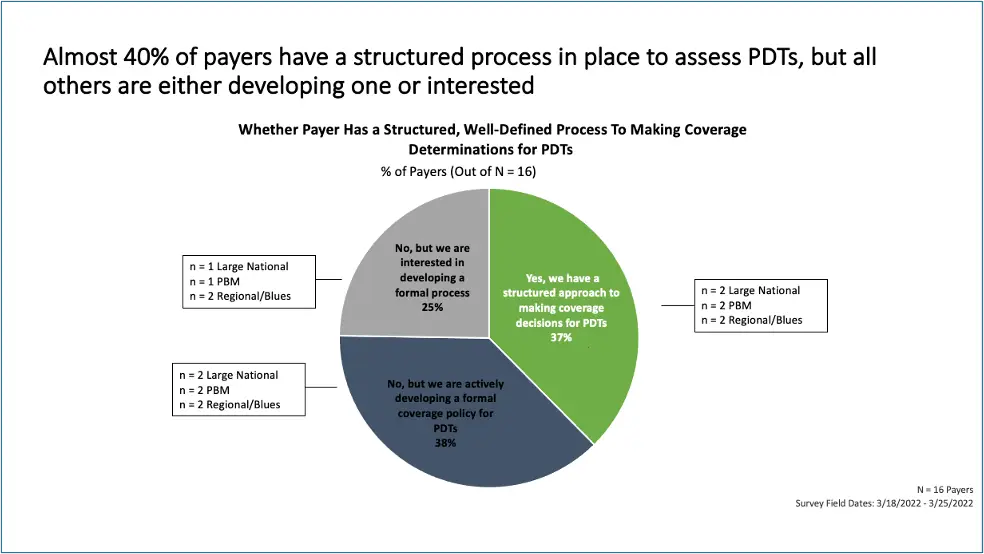
While it’s clear that payers are still hesitant to extend coverage to PDTs, incremental progress has been made. Payers might be dragging their feet on PDTs today, but ultimately, manufacturers need to prepare for an eventual shift: Nearly 40% of survey respondents have a structured process in place to assess PDTs, and 38% are actively developing a formal coverage policy for PDTs.
Also, in a bipartisan effort, senators from West Virginia, New Hampshire, Virginia, and California are rallying behind the Access to Prescription Digital Therapeutics Act of 2022, which would expand Medicare coverage to include PDTs and ensure they’re tested for safety and efficacy in randomized clinical trials, evaluated by FDA, and prescribed by healthcare professionals.
The industry is waiting to see what will happen with this legislative effort, but in the meantime, manufacturers with PDTs coming to market can focus on providing clinical evidence that supports improved outcomes, offering a great experience for patients and, ultimately, reducing costs for the payer. Moreover, those who lay the right groundwork—demonstrating clinical benefits for patients and value for the payer—will be well-equipped to seek out value-based contracting.
I know that I am far from the only parent or caregiver who has become frustrated by a lack of accessibility to promising new treatments. And while our survey findings reinforce that current PDT coverage is wholly inadequate for meeting patients’ needs, I’m confident that progress will be made—and quickly. Once the industry catches up to the many promising developments in this field, patients like my stepson will be able to access the therapy they need and deserve.






